
Holistic Hysterectomy Care for Women in Midlife
Expert coaching to support hysterectomy preparation and recovery by addressing pelvic floor health, hormones, nervous system regulation, and the realities of midlife healing.
Hysterectomy is one of the most common surgeries, yet for many women, it becomes one of the most confusing and unsupported transitions they’ve ever experienced.
If you feel unclear about what to expect before surgery or lost after being told to “listen to your body,” you’re not alone. This work bridges the gap between surgical care and real-life recovery.
Many women are surprised by how little guidance they received before and after hysterectomy.
You may have been told the surgery was routine.
That healing takes 6 weeks.
To “listen to your body,” avoid lifting and call if you have a fever.
And yet you might be thinking:
I don’t know what’s normal.
No one told me it would feel like this.
Why am I so exhausted?
How does this affect my pelvic floor, my hormones, or my sex life?
I was already in perimenopause, what does this change?
If you feel unprepared for hysterectomy, You’re not Alone.
These questions come up for many women, often quietly. They’re understandable, and the deserve thoughtful, real answers and guidance.

A complimentary call to see if support is a good fit.
Hysterectomy isn’t just a surgical event. It’s a whole-body and whole-life transition.
In midlife, your body is already adapting to hormonal shifts, changing energy levels, and evolving needs. Surgery adds another layer and can affect:
The pelvic floor and core system
Scar tissue, fascia and other connective tissue
Breathing mechanics and posture
The nervous system and energy regulation
Gut health and digestion
Hormonal balance and symptoms
Emotional well-being, identity and sexual health
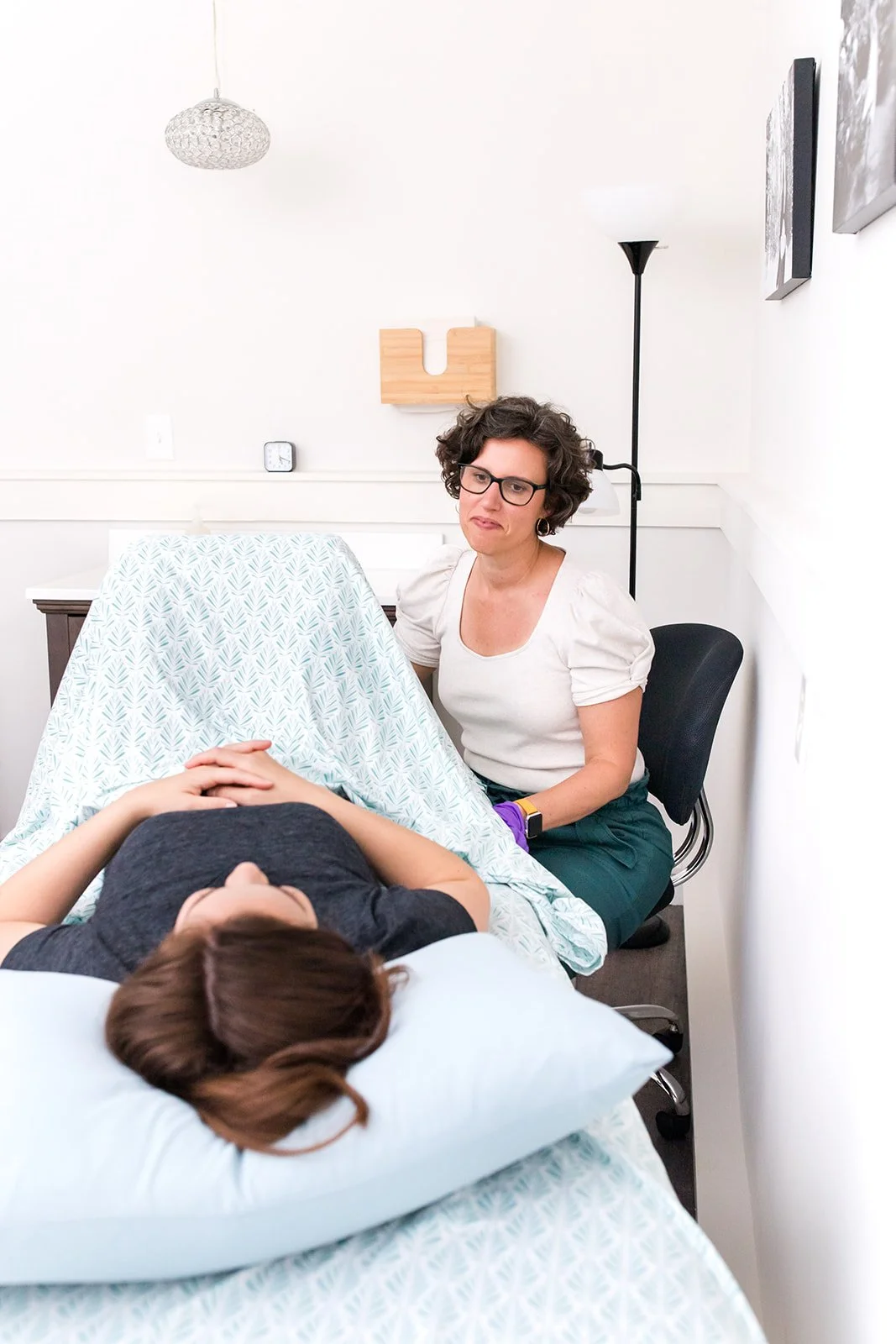
Why Hysterectomy can feel so hard —especially in midlife
When recovery focuses only on incision healing, you might be left feeling confused, unsure of how to move, and disconnected from your body.
This doesn’t mean something is wrong with you.
It means your recovery deserves a more complete approach.
Holistic Hysterectomy Recovery means supporting the whole woman, not just the surgical site. It recognizes that healing happens on multiple levels and unfolds over time.
I approach hysterectomy recovery through my simple framework I call “The Whole Woman Method.” It’s a way of making sense of what your body actually needs, when it needs it, and how to support long-term health instead of just getting though recovery.
What holistic hysterectomy recovery means here.

1: root
This phase focuses on establishing a steady foundation.
It involves understanding what was impacted during surgery, supporting the pelvic floor and core, calming the nervous system, and using rest, nutrition and breath to support the healing process.
2: Restore
This phase is about healing and rebuilding with intention.
It involves tissue healing, scar mobility, strength, mobility, and energy while also addressing hormonal shifts, digestion, sleep, and emotional processing.
Move forward without fear of overdoing it, or feeling stuck between resting and pushing.
3: resilience
This phase focuses on long-term confidence, capacity, and trust in your body.
It involves returning to exercise, building strength, reclaiming intimacy, and resuming life with clarity rather than hesitation.
Ready to do things differently?
A complimentary call to see if support is a good fit.
“I tell everyone that the biggest support in my hysterectomy healing journey was working with Allison Poole . She has changed how I view my body, my relationship with my body, and how I can move from either fear or ease and breath. She has supportive insights and so many tools to support every stage of healing. I am truly grateful to have her guidance.”
— Anna“Eight weeks after my hysterectomy, I went back to work still in daily pain. Eight months later I found Allison — and within 5 months of working together I was completely pain-free. She listened, she knew exactly what to do, and I looked forward to every session. It was absolutely the best thing I did for my healing and for protecting my pelvic floor long-term..”
— Linda
" Just 6 weeks out of a hysterectomy, I was in physical discomfort and my mobility was more limited than I imagined. Her holistic approach of education and physical therapy supported me tremendously to come out of my experience with information and an understanding of how I could accelerate my healing. She is such a valuable resource and I highly recommend her for her combination of warmth and expertise."
— E.S.
“Allison is kind, warm, and incredibly clear in her explanations. Our sessions never felt rushed, and I finally got answers to questions other providers had brushed past. Not only did I physically heal, I started to mentally heal too. If you're navigating hysterectomy recovery and feeling like something is missing, working with Allison is the piece you didn't know you needed.”
— Emily

Ways to work with me
Currently, I offer individualized support designed to meet you where you are, whether you are preparing for hysterectomy, recovering, or years out and still feeling off.
-
This is personalized coaching focused on helping you make sense of what your body is experiencing and how to support it through this transition.
1:1 support may include:
Guidance through preparation or recovery using the Root, Restore, Resilience framework
Education around pelvic floor health, core support, scar care, and movement
Support navigating fatigue, nervous system overwhelm, and energy changes
Hormonal and midlife health considerations, including perimenopause and menopause
Space to address emotional, identity, and sexual health concerns
Clear next steps
Sessions take place virtually and are individualized and collaborative, with the goal of helping you feel informed, supported, and confident in your body again.
-
For women located in Maine, 1:1 support can include a hybrid approach that combines coaching with in-person physical therapy.
This option allows for:
Hands-on pelvic health assessment and treatment
Integrated coaching to support recovery between visits
A whole-body approach that connects physical healing with lifestyle, nervous system, and long-term wellbeing
This hybrid model is ideal for women who want both guidance and hands-on support as they move through recovery.
If you’re not sure where to start, the free recovery guide is a good first step.

I bring together clinical expertise and compassionate coaching to guide women through this transition.
Over 22 years of clinical experience
More than a decade specializing in pelvic health
Advanced training in hysterectomy care, nutrition and hormonal health
Certification in therapeutic health coaching
Surgeons focus on the success of the procedure. I focus on how that procedure affects the rest of your body and life.
I’m here to help you understand what’s changed, what your body needs now, and how to move forward with confidence instead of guesswork.
Frequently Asked Questions
Still have questions? An Introductory Call is a great place to start.
-
The standard answer is 6 weeks, and while that's roughly when many women are cleared to return to normal activities, it doesn't reflect how long full recovery actually takes. Fatigue, pelvic heaviness, core weakness, hormonal and emotional shifts can linger for months, and that's completely normal. True recovery, where you feel strong, confident, and like yourself again, often unfolds over 6 to 12 months or more.
-
Persistent fatigue after hysterectomy is one of the most common things women mention, and one of the least talked about. Surgery is a significant physiological event. Add in hormonal changes, disrupted sleep, nervous system stress, and the emotional weight of navigating recovery with little guidance, and exhaustion makes complete sense. Fatigue that lingers well past the initial recovery window is often a signal that the body needs more support, not more willpower.
-
Yes, and this surprises a lot of women. The pelvic floor is directly connected to the structures involved in hysterectomy. Depending on the type of surgery, the support ligaments, surrounding fascia, and nerve pathways can all be affected. Some women notice changes in bladder or bowel function, pelvic pressure, or core stability. Others feel disconnected from that part of their body altogether. Pelvic floor rehabilitation is one of the most valuable things you can do after hysterectomy.
-
This depends on whether your ovaries were removed alongside your uterus. If the ovaries were kept, hormone production continues, though surgery can sometimes affect ovarian function. If the ovaries were removed, surgical menopause begins immediately, which brings a more abrupt hormonal shift than the gradual transition of natural menopause. Either way, hysterectomy during perimenopause adds complexity. Understanding what changed hormonally, and how to support your body through it, is a core part of holistic recovery.
-
Absolutely, and yes. Changes in sensation, lubrication, libido, and comfort during sex are common after hysterectomy, particularly when hormonal shifts are involved. These changes are real and they deserve honest conversation. They're also often very addressable with the right support. This is one of the things women most frequently tell me they wished someone had talked to them about sooner.

Don’t Miss Out!
Want to be the first to know about upcoming workshops, fresh blog posts, and exclusive midlife wellness tips? Join my email list and stay in the loop—because support, insight, and inspiration are just a click away.
